Sleep issues have become a widespread health concern in society. Studies indicate that 35.5% of American adults get less than 7 hours of sleep per night.
Importantly, not everyone who is sleep-deprived has insomnia.
I. Don’t Confuse “Sleep Deprivation” with “Insomnia”
Sleep deprivation is not the same as insomnia. Medically, sleep deprivation refers to having the capacity for sufficient sleep but not allowing oneself the opportunity to get enough sleep.
In contrast, insomnia involves sufficient opportunity but a lack of ability to sleep. Thus, even given adequate time (8 hours or more), those with insomnia cannot achieve sufficient sleep.
We’re discussing the latter here—insomnia.
II. What Type of Insomnia Do You Have?
Insomnia isn’t just about difficulty falling asleep. It can be classified into two types:
(1) sleep-onset insomnia, which is trouble falling asleep;
(2) sleep maintenance insomnia, which involves difficulty staying asleep.
These two types aren’t mutually exclusive. A person might experience one or both.
III. Self-Check: if you are suffering from insomnia
Research shows that one in five American adults exhibits symptoms of insomnia. While you might experience temporary insomnia due to job stress or a breakup, not all cases lead to an insomnia diagnosis, which adheres to strict medical criteria.
Here’s a self-checklist for insomnia:
- Dissatisfaction with sleep quantity or quality (such as difficulty falling asleep, interrupted sleep, or waking too early)
- Significant distress or impairment in daily activities
- Occurrence of sleep difficulties at least three nights a week for over three months
- Absence of other mental disorders or medical conditions that could affect sleep
If you meet all these criteria, you are likely suffering from insomnia. If unsure, it’s advisable to consult a sleep medicine specialist.

IV. Why is Falling Asleep Hard for You?
Several factors can make it difficult to fall asleep, including environmental, physical, and psychological aspects.
Setting aside external factors like inappropriate temperature, noise, and light, as well as physical aspects like age and illness. The most common contributors to chronic insomnia are psychological:
(1) emotional distress or worries;
(2) low mood or anxiety.
Fight-or-Flight mode
Thus, researchers continually study the biological bases of emotional fluctuations, identifying overactivity of the sympathetic nervous system as a key player of insomnia.
Throughout the long course of human evolution, when faced with threats or sudden stress, the sympathetic nervous system kicks in to trigger a sensible fight-or-flight response.
This causes physiological changes: an increase in heart rate, greater blood flow, elevated metabolic rate, and the release of stress hormones like cortisol and adrenaline, as well as activation of the brain’s alert areas.
These changes are beneficial when truly in danger or under threat. However, when you are lying in the comfort of a safe and cozy bed, the fight-or-flight mode becomes a disaster.
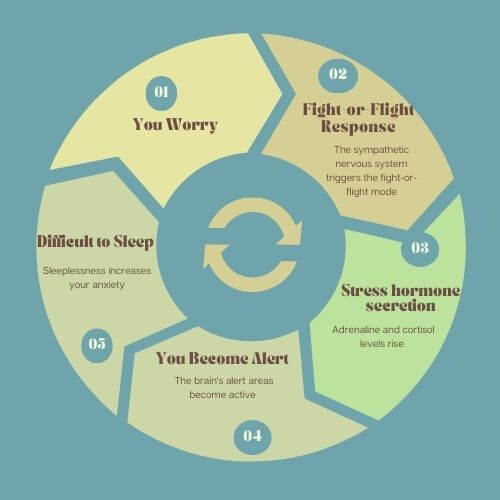
How Your Worry Destroy Your Sleep
Lying in bed, unable to sleep and laden with stress and worry, your body perceives these as signs of external danger, activating the sympathetic nervous system to initiate the fight-or-flight response.
The more anxious and unsettled you feel, the more excited your sympathetic nervous system becomes. This results in higher levels of adrenaline and cortisol, which further stimulate the alert regions of your brain, making it progressively harder to fall asleep.
This forms a vicious cycle:
>> You worry
>> The sympathetic nervous system triggers the fight-or-flight mode
>> Adrenaline and cortisol levels rise
>> The brain’s alert areas become active
>> You find it difficult to sleep
>> Your sleeplessness increases your anxiety…
V. Things You Can Do When you’re struggling to Fall Asleep
Knowing the physiological response caused by psychological factors, which creates a vicious cycle, how can we stop this relentless machinery of the brain?
Sleep Meditation
While sleep medications are commonly used to sedate the alert areas of the brain to facilitate sleep, their side effects are increasingly recognized, and they are not considered a reliable and safe option.
Cognitive Behavioral Therapy (CBT)
Recently, non-pharmacological treatments for insomnia, like Cognitive Behavioral Therapy for Insomnia (CBT-I), have gained prominence as first-line treatments. They break poor sleep habits and address sleep-blocking anxiety.
Sleep-enhancing tips
Apart from professional help, insomnia sufferers can reduce caffeine and alcohol intake, eliminate sleep disturbances, and follow these sleep-enhancing tips:
- Maintain regular sleep times, even on weekends.
- Go to bed only when sleepy and avoid napping on the couch early in the evening.
- If unable to sleep, get up and engage in quiet activities until sleepiness returns.
- Avoid napping during the day if nighttime sleep is difficult.
- Learn to relax before going to bed to reduce anxiety-inducing thoughts and worries.
- Keep visible clocks out of the bedroom to avoid anxiety from clock-watching.
If there’s one piece of advice you should follow, it’s this one: go to bed and wake up at the same time every day. It is crucial for establishing a stable biological clock.
Moreover, based on personal experience, if you can’t sleep, don’t force yourself. Instead, embrace the situation with a mindset of surrender—”So be it!” You may fall asleep soon after that.
